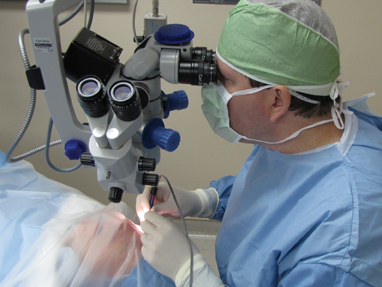
Treating Cataracts
What is a Cataract?
A cataract is an eye disease in which the clear lens becomes becomes cloudy or opaque, causing a decrease in vision. This clouding of the lens caused by cataract formation causes distorted vision. Cataracts usually occur gradually during the normal aging process but can sometimes develop rapidly. In rare cases, cataracts can be present at birth or in early childhood.
Most cataracts appear to be caused by changes in the protein structure within the lens. There are also potential environmental causes including excessive ultraviolet light exposure, exposure to ionizing radiation, diabetes, smoking or the use of certain medications.
Symptoms of a Cataract
Cataracts can cause negative visual changes, including blurred vision, difficulty with glare, dull color vision, increased nearsightedness and even double vision. A change in glasses may help for some period, but as the cataract becomes more dense vision will deteriorate and strong glasses or contact lenses will no longer help. Cataracts do not normally cause pain or obvious discomfort until they become very advanced.
Diagnosis of Cataracts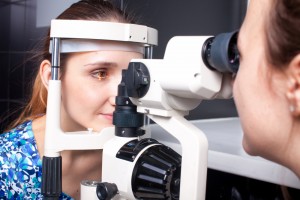
Cataracts are identified through an eye examination, when an eye care professional identifies and abnormal lens. The lens is viewed through specialized instruments. Using a variety of tests – including visual acuity, glare sensitivity, color vision and contrast sensitivity – the doctor will assess how much the cataract is affecting vision. Your doctor will provide the patient treatment options, including surgery. Surgery is recommended for people who are experiencing meaningful loss in vision and are symptomatic secondary to cataract.
Types of Cataract Surgery
Cataract surgery is normally performed in a out patient setting, with minimal sedation. It does not put significant stress on the patient’s heart or lungs. As cataracts are a medical condition, procedures are normally covered in part or full by insurance companies. There are three basic techniques for cataract surgery.
Phacoemulsification: Using an operating microscope, the surgeon makes a very small incision in the surface of the eye in or near the cornea. A thin ultrasound probe is inserted into the eye and uses ultrasonic vibrations to dissolve the clouded lens. The tiny pieces are then suctioned out through the probe. Once the cataract is removed, and artificial lens is placed into the capsular bag; the lens is critical to help your eye focus after surgery.
Extracapsular cataract surgery: This procedure is normally used to address advanced cataracts. This process requires a larger incision, allowing the cataract to be removed in one piece. Like Phacoemulsification, an artificial lens is placed in the capsular bag. This surgery requires a number of sutures to close the wound and visual recovery is often slower.
Intracapsular cataract surgery: This surgical technique requires a larger incision, with the surgeon removing the entire lens and and the surrounding capsule together. The intraocular lens is placed in front of the iris. This technique is not commonly used but can be effective in cases of significant trauma.
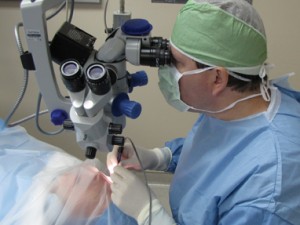 Cataract Surgery – What to Expect
Cataract Surgery – What to Expect
Prior to surgery, your ophthalmologist will discuss the surgery process and perform a medical exam. She will review the medications to avoid prior to surgery. Most cataract surgeries will be performed in a surgery center of hospital. Most surgeries are done on an outpatient basis, with minimal sedation.
The actual procedure will take about 20 minutes. A anesthesiologist will work with the ophthalmologist the type of sedation to be used. While the cataract surgery is not normally painful, medications will be used to alleviate discomfort. After the surgery, you will be placed in a recovery room. The surgeon will examine you and prescribe eyedrops that you will need to take for a few weeks, to help protect against infection and inflammation.
Following surgery, you will return to visits to the doctor within the first few days and for the first few weeks. The doctor will monitor for any complications. Within several days, you should notice improved vision. You doctor will fit you with glasses, if needed. Once your vision has stabilize, you will be allowed to resume normal activities.
Cataract surgery is a very safe procedure, with a high success rate; however, in rare cases complications can occur. These complications can include persistent inflammation, changes in eye pressure, infection or swelling of the retina at the back of the eye. Your ophthalmologist will identify complications in the post surgery follow-up and address with standard protocol.
To learn more about cataracts and cataract surgery options, schedule a consultation with our experts at White Plains Eye Surgery.